Abstract
Introduction:
Aggressive non-Hodgkin's lymphoma (aNHL) with secondary central nervous system (sCNS) involvement has a poor prognosis. Studies have reported a response to induction treatment as low as 35%, leaving less than half of patients eligible for autologous stem cell transplant (ASCT). Outcomes of patients in these clinical scenarios are dismal and treatment is ill-defined. Small case series suggest chimeric antigen receptor (CAR)-T cell therapy may play a role in the management of relapsed/refractory (R/R) B-cell lymphoma (BCL) with sCNS involvement, but follow-up is limited and response duration is uncertain. Allogeneic hematopoietic stem cell transplant (alloHCT) offers a durable remission for a subset of patients with R/R systemic aNHL primarily mediated through a graft versus lymphoma (GVL) effect, but it is unclear if GVL properties include the immune-privileged CNS. The present study aims to describe outcomes of a cohort of patients with R/R aggressive B- and T-cell NHL with sCNS involvement who underwent alloHCT at a single academic institution.
Methods:
This is a retrospective analysis that includes all patients with R/R aNHL with sCNS involvement who underwent alloHCT at the University of California, Los Angeles from 2005-2020. The UCLA Institutional Board Review approved this study. Relevant clinical data was extracted from medical records. Hematopoietic cell transplantation comorbidity index (HCT-CI) and time to neutrophil and platelet engraftment were measured according to Center for International Blood and Marrow Transplant Research criteria.
Results:
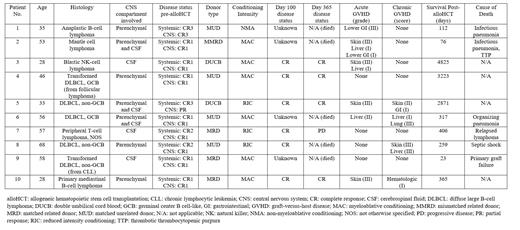
Ten patients were included (3 females, 7 males). Histologic subtypes included anaplastic BCL (1), mantle cell lymphoma (1), blastic natural killer-cell lymphoma (1), peripheral T-cell lymphoma, not otherwise specified (1), primary mediastinal BCL (1), and diffuse large B-cell lymphoma (DLBCL) (non-germinal center=3, germinal center-like=2). Two DLBCL patients had histologic transformed lymphoma (follicular lymphoma =1, chronic lymphocytic lymphoma = 1). Four patients had sCNS involvement at the time of initial diagnosis or during frontline treatment; the remaining 6 patients developed sCNS lymphoma at relapse. sCNS lymphoma was identified in the parenchymal (n=4), leptomeningeal (n=3), or both (n=3) compartments.
The median age at the time of alloHCT was 49.5 (range 28-68), and 1 patient was ˃ 60. At the time of alloHCT, 1 patient had residual disease in the CNS and the remaining 9 patients were in a complete remission. Eight patients received ˃ 3 prior lines of therapy, and 3 patients failed prior ASCT. HCT-CI scores were 0 (n=1), 1 (n=2), 2 (n=3), 3 (n=1), and unknown (n = 3). Donor types included 10/10 matched related (3), 10/10 matched unrelated (4), 9/10 mismatched related (1), and double umbilical cord blood (2). Graft source was peripheral blood in 8 patients and cord blood in 2 patients. Conditioning regimens included myeloablative, reduced intensity and non-myeloablative in 6, 3 and 1 patient(s), respectively. Six patients received total body irradiation-containing conditioning. The average time to neutrophil engraftment was 18 days (range 11-29), and the average time to platelet engraftment was 26.5 days (range 18-59). One patient had primary graft failure.
Of the 6 patients with day 100 disease reassessment (CR at time of alloHCT=5, PR in CNS at time of alloHCT=1), all were in CR. With a median follow-up of 341 days, 2 patients relapsed (CNS=1 and systemic = 1), and 6 patients died. Cause of death included infection (n=3), lymphoma (n=1), primary graft failure (n=1), and organizing pneumonia (n=1). Six patients developed acute graft versus host disease (GVHD) (grade 1-2, n=1; grade 3, n=5), and 4 patients developed chronic GVHD (score 1-2, n= 2; score 3, n=2). The median overall and progression-free survival for the entire cohort was 341 days (range 23-4825) and 268.5 days (range 23-4825), respectively.
Conclusions:
AlloHCT in patients with R/R aNHL with sCNS involvement is feasible and may provide a durable response in a subset of patients. Four patients remained alive and free of disease one year post-alloHCT and one patient converted from a PR to a CR in the CNS 100 days post-alloHCT, suggesting effective donor immune surveillance within the CNS. Transplant-related morbidity and mortality limits the widespread application of this therapeutic modality and less toxic approaches are urgently needed.
No relevant conflicts of interest to declare.